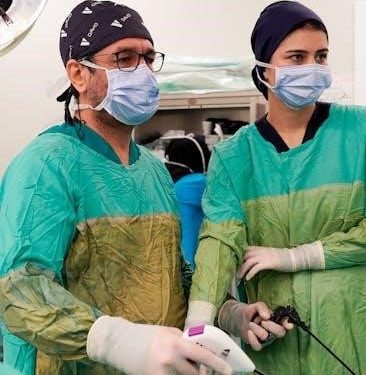
Laparoscopic cholecystectomy, a minimally invasive surgical procedure, revolutionized gallbladder removal since its recognition in 1987, offering a less traumatic alternative to open surgery.
This technique utilizes small incisions and a camera, providing enhanced visualization and quicker recovery times for patients experiencing gallbladder-related issues like cholecystitis.
The procedure is a common treatment for gallbladder inflammation, and advancements like single-site surgery (LESS) further refine the cosmetic and recovery aspects.
Guidelines and comparisons of access techniques continually optimize this widely accepted and effective surgical approach for gallbladder disease management.
Historical Context of Laparoscopic Surgery
Laparoscopy emerged as a pivotal surgical advancement during the 20th century, fundamentally altering the landscape of surgical interventions. Initially employed for diagnostic purposes, its potential for therapeutic procedures quickly became apparent. The first documented laparoscopic cholecystectomy, performed by Phillipe Mouret in 1987, marked a watershed moment, transitioning the procedure from experimental to established practice.
Prior to this breakthrough, gallbladder removal necessitated large abdominal incisions, leading to prolonged recovery periods and increased patient discomfort. The introduction of laparoscopy offered a significantly less invasive alternative, utilizing small incisions through which a camera and specialized instruments could be inserted.
This innovation dramatically reduced postoperative pain, shortened hospital stays, and facilitated a faster return to normal activities. The rapid adoption of laparoscopic cholecystectomy demonstrated the transformative power of minimally invasive techniques, paving the way for the widespread application of laparoscopy across various surgical specialties.
Further refinements, such as single-site laparoscopy (LESS), continue to build upon this legacy, emphasizing cosmetic benefits and enhanced patient outcomes.
Advantages of Laparoscopic Approach
Laparoscopic cholecystectomy presents numerous advantages over traditional open surgery, establishing it as the preferred method for gallbladder removal. Primarily, the minimally invasive nature of the procedure results in significantly reduced postoperative pain, allowing for earlier mobilization and a quicker return to daily activities.
Smaller incisions translate to less scarring, improving cosmetic outcomes and enhancing patient satisfaction. Hospital stays are typically shorter, decreasing healthcare costs and minimizing the risk of hospital-acquired infections.
Enhanced visualization provided by the laparoscopic camera allows for precise dissection and identification of critical anatomical structures, potentially reducing the risk of complications.
Furthermore, the technique often leads to a faster recovery period, enabling patients to resume their normal routines sooner. Advancements like single-site surgery (LESS) amplify these benefits, offering even better cosmesis with a single, hidden scar.
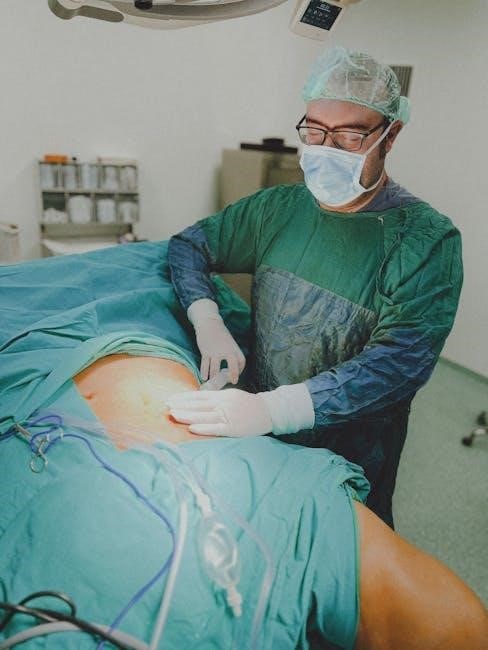
Preoperative Preparation
Comprehensive evaluation, including medical history and imaging like ultrasound or CT scans, is crucial before laparoscopic cholecystectomy.
Informed consent, detailing potential risks, is essential for patient understanding and shared decision-making prior to the surgical intervention.
Patient Evaluation and Medical History
A thorough patient evaluation is the cornerstone of preoperative preparation for laparoscopic cholecystectomy. This begins with a detailed medical history, focusing on symptoms like abdominal pain, nausea, and vomiting, specifically related to potential gallbladder issues.
The surgeon will inquire about pre-existing conditions such as cardiac disease, pulmonary problems, diabetes, and bleeding disorders, as these can influence surgical risk and anesthetic considerations.
Medication review is vital, with particular attention to anticoagulants or antiplatelet drugs that may need adjustment before surgery to minimize bleeding complications.
Allergies, especially to medications or latex, must be documented. Previous surgical history, including any prior abdominal surgeries, is also important, as it can affect port placement and dissection techniques.
Finally, a physical examination is performed to assess the patient’s overall health status and identify any potential contraindications to surgery.
Imaging Studies (Ultrasound, CT Scan)
Diagnostic imaging plays a crucial role in confirming the diagnosis and guiding surgical planning for laparoscopic cholecystectomy. Ultrasound is typically the first-line imaging modality due to its non-invasive nature, accessibility, and ability to visualize gallstones and gallbladder wall thickening.
However, CT scans may be necessary in cases where ultrasound findings are inconclusive or to evaluate for complications such as perforation or abscess formation. CT scans provide a more detailed anatomical view of the gallbladder and surrounding structures.
These scans help determine the severity of cholecystitis and rule out other potential causes of abdominal pain.
Furthermore, imaging can identify anatomical variations that may influence the surgical approach. Preoperative imaging aids in assessing the patient’s suitability for laparoscopic surgery and anticipating potential challenges during the procedure.
Accurate imaging interpretation is essential for safe and effective surgical management.
Informed Consent and Risk Discussion
Obtaining informed consent is paramount before proceeding with laparoscopic cholecystectomy. This process involves a thorough discussion with the patient regarding the surgical procedure, its benefits, potential risks, and alternative treatment options.
Patients must understand the nature of the surgery, including the use of small incisions, camera insertion, and gallbladder removal. Potential risks, such as bile duct injury, bleeding, infection, and anesthesia-related complications, must be clearly explained.
The surgeon should also discuss the possibility of conversion to open surgery if necessary;
Realistic expectations regarding postoperative pain, recovery time, and dietary modifications are crucial.
Documented consent signifies the patient’s understanding and voluntary agreement to undergo the procedure. A comprehensive discussion ensures patient autonomy and fosters a trusting doctor-patient relationship.
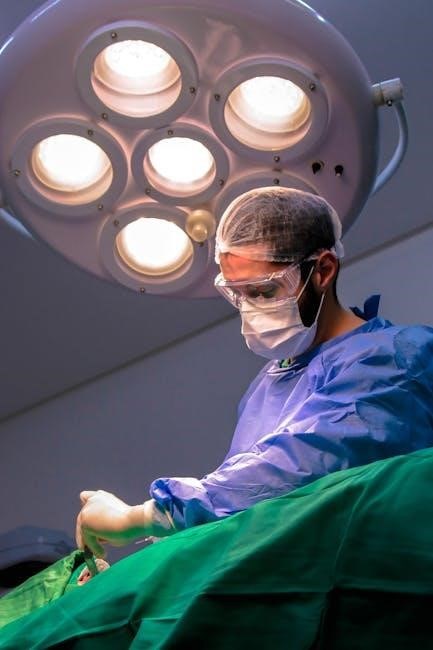
Surgical Procedure Steps
Laparoscopic cholecystectomy involves precise steps: anesthesia, port placement, camera insertion, dissection of Calot’s triangle, and careful identification of vital structures.
Clipping and division of the cystic duct and artery precede gallbladder removal, ensuring a safe and effective procedure for optimal patient outcomes.
Anesthesia and Patient Positioning
General anesthesia is universally employed for laparoscopic cholecystectomy, ensuring complete patient comfort and muscle relaxation throughout the procedure. This allows the surgical team optimal access and control.
Patient positioning is crucial for successful surgery. Typically, the patient is placed in a supine position on the operating table, with arms extended, often secured with arm boards.
A slight reverse Trendelenburg position – elevating the head and lowering the legs – is frequently utilized to facilitate visualization of the gallbladder and surrounding structures.
Careful padding is applied to pressure points to prevent nerve damage or skin breakdown. The abdomen is prepped and draped in a sterile fashion, creating a wide surgical field.
Proper positioning minimizes strain on the patient and optimizes the surgeon’s ergonomic comfort, contributing to a safer and more efficient laparoscopic cholecystectomy.
Port Placement Techniques
Port placement is a fundamental aspect of laparoscopic cholecystectomy, dictating instrument access and surgical efficiency. A standard four-port technique is commonly used, though variations exist.
Typically, a 10-12mm umbilical port is established first, serving as the entry point for the camera. Additional ports – usually 5mm – are then inserted under direct visualization, strategically positioned to allow triangulation and optimal instrument maneuverability.
Common locations include the right subcostal region, the epigastric region, and the right midclavicular line. Precise placement considers the patient’s anatomy and the surgeon’s preference.
Access-port diameters are carefully selected to balance instrument functionality with minimizing abdominal wall trauma. Newer techniques, like single-site laparoscopy (LESS), utilize a single incision for all instruments.
Secure port placement is vital to maintain pneumoperitoneum and prevent carbon dioxide leakage, ensuring a stable surgical field throughout the procedure.
Insufflation and Camera Insertion
Insufflation, the introduction of carbon dioxide gas into the abdominal cavity, is crucial for creating the pneumoperitoneum – the working space for laparoscopic cholecystectomy. This is typically achieved via a Veress needle inserted through the umbilical incision.
Once adequate pressure (usually 12-15 mmHg) is established and confirmed, the trocar for the camera is inserted. The laparoscope, equipped with a light source and camera, provides a magnified view of the abdominal contents on a monitor.
Careful inspection of the abdominal cavity follows, assessing for any adhesions or anatomical variations. Proper insufflation is essential for optimal visualization and instrument manipulation.
Maintaining consistent pneumoperitoneum pressure throughout the procedure is vital. Insufficient pressure can compromise visualization, while excessive pressure may cause physiological stress.
The initial camera view guides subsequent port placement, ensuring safe and effective access for the surgical instruments.
Dissection of Calot’s Triangle
Dissection of Calot’s Triangle, a critical step, involves carefully exposing the cystic duct and cystic artery. This anatomical space is bordered by the cystic duct, common hepatic duct, and the inferior edge of the liver.
Sharp dissection, utilizing laparoscopic instruments, is employed to clear away connective tissue and fat, meticulously revealing the structures within the triangle. Gentle traction on the gallbladder assists in this process.
Precise identification of these vessels is paramount to avoid injury to the common bile duct. A thorough understanding of anatomical variations is essential for safe dissection.
Careful attention is paid to any aberrant anatomy or unusual vessel courses. This step demands meticulous technique and a clear surgical field.
Complete exposure of Calot’s Triangle allows for safe and accurate clipping and division of the cystic duct and artery, paving the way for gallbladder removal.
Identification of Cystic Duct and Artery
Identification of the cystic duct and artery is a pivotal moment in laparoscopic cholecystectomy, demanding meticulous attention to detail. Following Calot’s triangle dissection, these structures become visible.
The cystic duct, typically smaller in diameter than the common bile duct, connects the gallbladder to the biliary system. The cystic artery, branching from the right hepatic artery, supplies blood to the gallbladder.
Careful differentiation from the common bile duct is crucial to prevent bile leak or injury. Intraoperative cholangiography may be considered to confirm anatomy.
Gentle dissection and retraction are used to fully expose the vessels, allowing for clear visualization of their course and relationship to surrounding tissues.
Confirmation of anatomy is essential before proceeding to clipping and division, ensuring patient safety and minimizing the risk of postoperative complications;

Clipping and Division of Cystic Duct and Artery
Clipping and division of the cystic duct and artery represent a critical step, executed with precision to ensure hemostasis and prevent bile leakage. Titanium clips are typically applied to both structures.
At least two clips are placed on the cystic duct, and typically one or two on the cystic artery, ensuring secure occlusion. The clips should be positioned proximally, away from any potential bile duct or arterial branches.
Following clip application, the cystic duct and artery are divided between the clips using laparoscopic scissors or harmonic energy devices.
Careful inspection of the clip placement and division site is paramount to confirm complete occlusion and rule out any bleeding or bile leakage.
This step requires focused attention and a thorough understanding of biliary anatomy to minimize the risk of postoperative complications.
Gallbladder Dissection from Liver Bed
Gallbladder dissection from the liver bed is performed meticulously to minimize trauma and ensure complete removal. This stage follows cystic duct and artery ligation and division.
Dissection typically begins with grasping the gallbladder fundus and gently elevating it. Using laparoscopic instruments, the peritoneum surrounding the gallbladder is carefully incised, separating it from the liver surface.
Cauterization or harmonic energy may be employed to achieve hemostasis during dissection, addressing small bleeding vessels encountered along the liver bed.
Attention is given to identify and preserve any anatomical variations or adhesions that may be present, ensuring a clean and complete dissection.
Complete mobilization of the gallbladder from the liver bed is crucial for facilitating smooth extraction through the laparoscopic ports, avoiding any retained tissue.
Gallbladder Extraction
Gallbladder extraction represents the final surgical step, requiring careful maneuvering to avoid injury to surrounding structures. Following complete dissection from the liver bed, the gallbladder is prepared for removal.
Typically, the gallbladder is placed into an endoscopic retrieval bag to contain bile and prevent spillage into the abdominal cavity, minimizing postoperative complications like peritonitis.
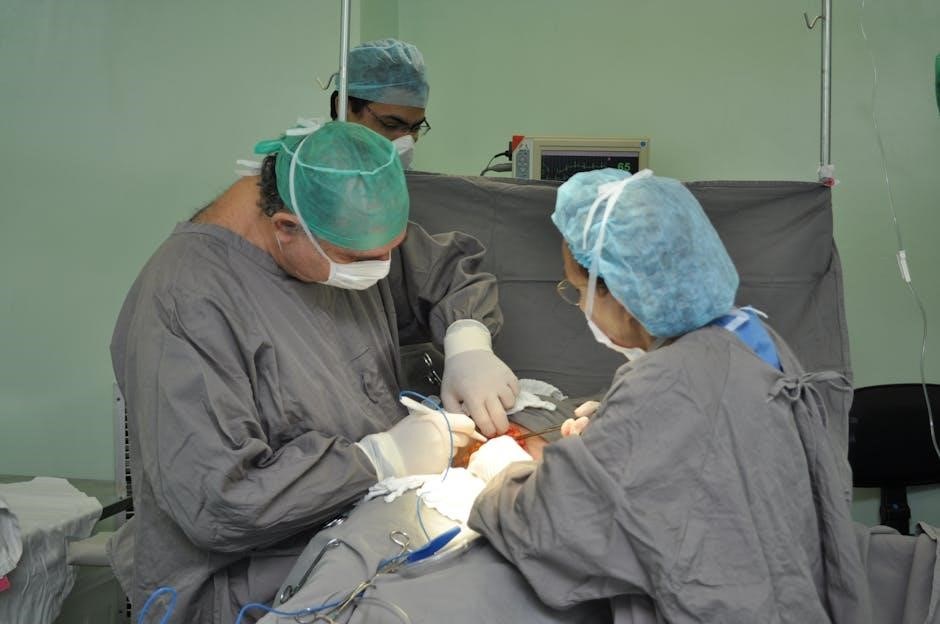
The bag is then carefully extracted through one of the port sites, often the umbilical port, which may require slight enlargement to accommodate the specimen.
Gentle traction and controlled movements are essential during extraction to prevent damage to the port site fascia or abdominal wall muscles.
Once the gallbladder is removed, a thorough inspection of the surgical bed is performed to confirm hemostasis and rule out any retained stones or bile leaks, completing the procedure.
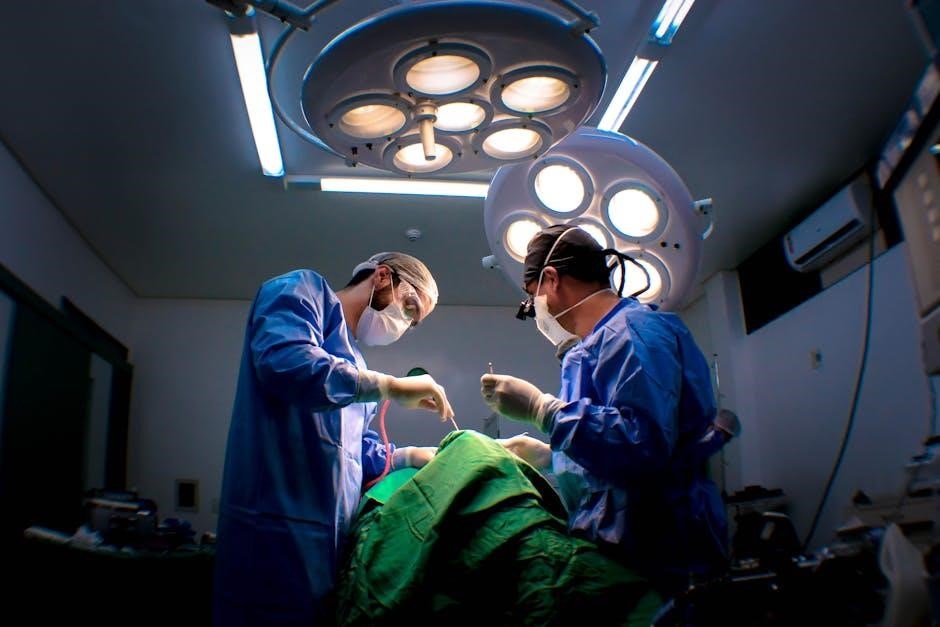
Postoperative Care
Postoperative care focuses on pain management, dietary progression, and wound healing following laparoscopic cholecystectomy, ensuring a smooth recovery for the patient.
Patients receive guidance on dietary recommendations and wound care, alongside scheduled follow-up appointments to monitor their progress.
Pain Management
Effective pain management is crucial following laparoscopic cholecystectomy, significantly impacting patient comfort and recovery speed. Initially, pain is typically managed with intravenous or oral analgesics, tailored to the individual’s needs and pain level.
Patients are often transitioned to oral pain medications, such as nonsteroidal anti-inflammatory drugs (NSAIDs) or opioid analgesics, for continued relief at home.
Shoulder pain, a common side effect due to carbon dioxide gas used during the procedure, can be managed with simple analgesics and gentle movement.
Healthcare providers emphasize the importance of adhering to the prescribed pain medication schedule and communicating any persistent or worsening pain.
Non-pharmacological methods, like deep breathing exercises and relaxation techniques, can also complement medication for enhanced pain control and overall well-being during the postoperative period.
Dietary Recommendations
Post-laparoscopic cholecystectomy dietary guidelines focus on a gradual return to normal eating, starting with clear liquids immediately after surgery. This progression minimizes stress on the digestive system as it adjusts to the absence of the gallbladder.
Patients typically advance to a low-fat diet within a few days, avoiding fried, greasy, or heavily processed foods that can cause discomfort or diarrhea.
Small, frequent meals are recommended over large ones, easing the digestive process and preventing bloating.
Gradually reintroducing fiber-rich foods is important for maintaining regular bowel movements, but should be done cautiously to avoid initial discomfort.
While most individuals can tolerate a normal diet long-term, some may experience temporary changes in bowel habits or require ongoing dietary modifications to manage symptoms.
Wound Care and Follow-up
Postoperative wound care following laparoscopic cholecystectomy is generally straightforward. Small incision sites require keeping clean and dry, typically covered with simple bandages for a few days.
Patients should monitor for signs of infection, such as increased redness, swelling, drainage, or fever, and report these to their surgeon immediately.
Staples or sutures are usually removed or dissolve within 7-10 days, depending on the type used.
A follow-up appointment with the surgeon is scheduled within 1-2 weeks to assess healing, address any concerns, and discuss pathology results.
Activity restrictions are typically minimal, but strenuous activity and heavy lifting should be avoided for several weeks to allow for complete internal healing.
Regular check-ins ensure optimal recovery and early detection of any potential complications.
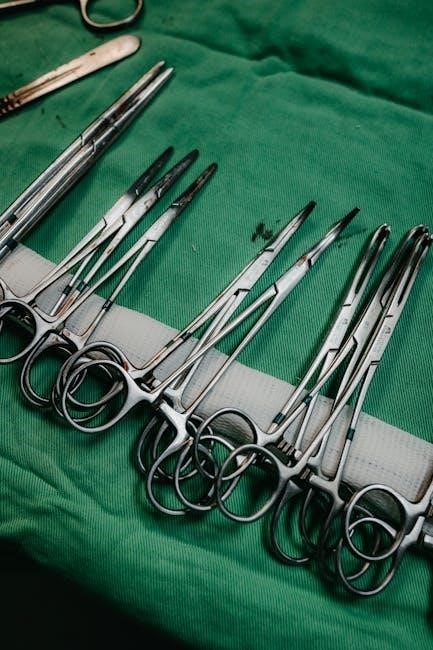
Potential Complications
Although rare, laparoscopic cholecystectomy carries risks like bile duct injury, bleeding, and infection; careful surgical technique minimizes these possibilities for patient safety.
Prompt recognition and management of complications are crucial for positive outcomes following gallbladder removal surgery.
Bile Duct Injury
Bile duct injury represents one of the most serious, though thankfully uncommon, complications associated with laparoscopic cholecystectomy. This can range from minor bile leaks to significant damage requiring complex reconstruction. The risk stems from the anatomical proximity of the cystic duct and common bile duct within Calot’s triangle, demanding meticulous dissection and identification.
During the procedure, misidentification of the anatomy, particularly in cases of inflammation or anatomical variations, can lead to inadvertent injury. Surgeons employ techniques like intraoperative cholangiography – an X-ray of the bile ducts – to help delineate the anatomy and reduce this risk.
If a bile duct injury is suspected, immediate conversion to open surgery may be necessary for repair. Delayed recognition can lead to peritonitis, sepsis, and long-term complications, emphasizing the importance of vigilance and appropriate post-operative monitoring for signs of bile leakage or obstruction.
Bleeding
Bleeding during or after laparoscopic cholecystectomy, while usually manageable, constitutes a potential complication. It typically arises from the cystic artery, gallbladder bed, or port sites. The laparoscopic approach, utilizing smaller incisions, generally results in less blood loss compared to open cholecystectomy, but careful hemostasis remains crucial throughout the procedure.
Precise clipping and division of the cystic artery and duct are paramount to prevent post-operative bleeding. Electrocautery is frequently employed to achieve hemostasis in the gallbladder bed. Significant bleeding requiring conversion to open surgery is rare but may occur if anatomical variations or inflammation obscure critical structures.
Post-operative bleeding can manifest as abdominal pain, distension, or signs of hypovolemic shock. Prompt identification and intervention, potentially including blood transfusion or re-operation, are essential to ensure patient stability and prevent further complications.
Infection
Infection represents a potential, though relatively uncommon, complication following laparoscopic cholecystectomy. The risk is minimized through meticulous surgical technique and adherence to sterile protocols. Wound infections can occur at the port sites, typically presenting as redness, swelling, and pain. Intra-abdominal infections, such as peritonitis or abscess formation, are rarer but more serious.
Prophylactic antibiotics are often administered pre-operatively to reduce the bacterial load and decrease the incidence of post-operative infections. Thorough irrigation of the surgical site during the procedure helps eliminate potential contaminants. Bile spillage, if it occurs, increases the risk of intra-abdominal infection.
Post-operative signs of infection necessitate prompt evaluation and treatment, which may include antibiotic therapy and, in severe cases, drainage of any abscesses. Careful wound care and monitoring for fever are crucial components of post-operative management.
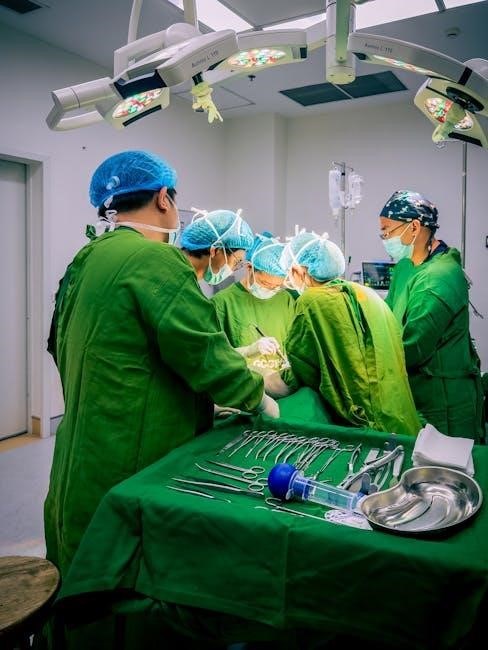
Single-Site Laparoscopic Cholecystectomy (LESS)
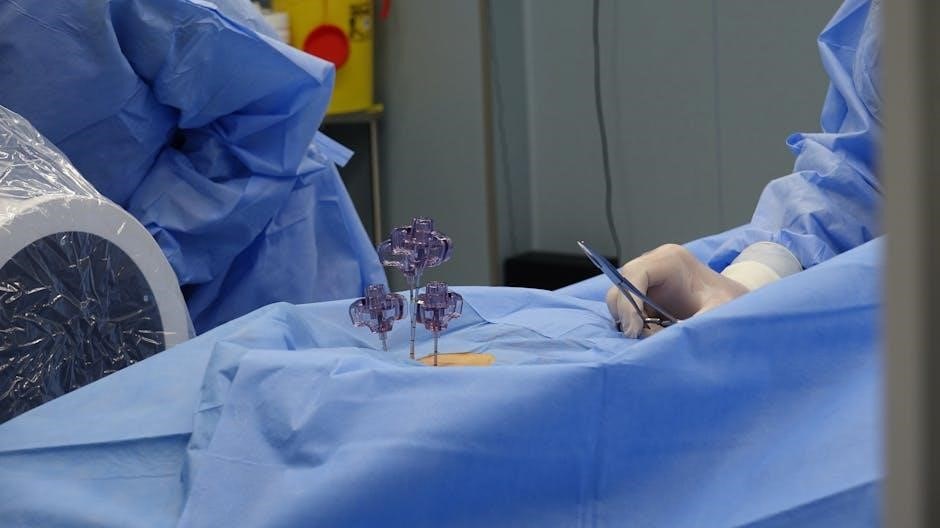
Laparoscopic Single-Site Cholecystectomy (LESS) represents an evolution of traditional laparoscopic techniques, aiming to further minimize invasiveness. This approach utilizes a single incision, typically within the umbilicus, through which all surgical instruments and the camera are inserted.
LESS offers cosmetic advantages, resulting in a single, concealed scar instead of multiple smaller incisions. However, it presents technical challenges due to instrument crowding and limited triangulation. Specialized instruments and advanced surgical skills are essential for successful LESS procedures.
While offering benefits like reduced post-operative pain and improved cosmetic outcomes, LESS isn’t suitable for all patients. Factors like body habitus and the complexity of the case influence suitability. It goes a step beyond conventional laparoscopic cholecystectomy, continually evolving with improved techniques.